 Français
Français Antibiotic Drugs
Metronidazole
Metronidazole is an antiprotozoal, antibacterial and antihelminthic nitroimidazole agent.
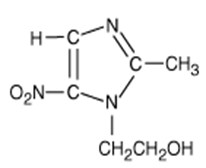
Chemical structure
The chemical formula is C6H9N3O3 and the molecular weight is 171.2.
Mechanism of action
Metronidazole is reduced to disrupt energy metabolism of anaerobes by hindering the replication, transcription and repair process of DNA results in cell death. Presence of oxygen prevents reduction of metronidazole and so reduces its cytotoxicity.
Pharmacokinetics
Plasma concentration and clearance of metronidazole is dose dependent. Reddish brown discoloration of urine in some patients may be due to the presence of unidentified pigments derived from the drug.
Antimicrobial spectrum
Metronidazole is active against T.vaginalis, E. histolytica, Giardia lamblia, Blastocystis hominis, Balantadium coli,spirochaetes and anerobic streptococci. Clostridia induced pseudomembranous colitis responds to metronidazole.
Indications, administration and dosage
Amoebiasis - Metronidazole is a first line drug for all forms of amoebic infection. For invasive dysentery and liver abscess-800 mg TDS (children 30-50 mg/kg/day) for 7-10 days.
Giardiasis - It is highly effective in a dose of 400 mg TDS for 7 days.
Trichomonas vaginitis – Metronidazole is drug of choice; 400 mg TDS for 7 days achieves nearly 100% cure.
Helicobacter pylori gastritis/peptic ulcer - Metronidazole 40 mg TDS.
Metronidazole is also useful in treatment of pseudomernbranous enterocolitis, ulcerative gingivitis, trench mouth.
Metronidazole sensitizes tumour cells for ionizing radiation but is not used clinically for this purpose.
Precautions, contraindications and warnings
Metronidazole is contraindicated in patients with prior history of hypersensitivity to metronidazole or other nitroimidazole derivatives, patients with neurological disease, blood dyscrasias and in first trimester of pregnancy. Disulfiram-type reaction can occur if metronidazole is received by alcoholics.
Adverse effects
Common side effects of metronidazole are nausea, vomiting, dry mouth, abdominal cramps, metallic taste, headache, anorexia. Other side effects include vomiting, diarrhea, rashes, furry tongue, glossitis, dizziness, vertigo, dysuria, cystitis.
Technical Description on Metronidazole
Metronidazole is an antiprotozoal drug but it is also active against bacteria and it belongs to the nitroimidazole group.
Chemical structure
Chemically it is 1-(beta-hydroxyethyl)-2-methyl-5-nitroimidazole.The chemical formula is C6H9N3O3 and the molecular weight is 171.2.

Preparations available
Oral: 375 mg capsules; 250 and 500 mg tablets; extended-release 750 mg tablets
Parenteral: 5 mg/mL
Mechanism of action
Metronidazole is not active by itself; its nitro group gets activated to convert it into the active form. This activation is done by the micro-organisms. It is selectively toxic to anaerobic and micro-aerophilic pathogens. After entering the cell by diffusion its nitro group is reduced by certain redox proteins functional only in anaerobic microorganisms to extremely reactive nitrogen radical that is cytotoxic. The nitro radical of metronidazole acts as an electron sink which competes with the biological electron acceptors of the anaerobic organism for the electrons produced by the pyruvate: ferrodoxin Oxidoreductase (PFOR) enzyme pathway of pyruvate oxidation. The energy metabolism of anaerobes is, thus, disturbed and replication, transcription and repair process of DNA is hindered leading to cell death. Metronidazole and oxygen both strive for the electrons formed during metabolism of energy. Hence oxygen decreases the cytotoxic action caused by metronidazole and also reduces its activation. Anaerobes which develop metronidazole resistance become deficient in the mechanism that generates the reactive nitro radical from it.
Antimicrobial activity
Metronidazole has activity against many of the obligate group of anaerobes. Anerobic bacteria which are facultative, aerobic and non-sporulating gram-positive bacilli are mostly resistant.
- Metronidazole has direct trichomonacidal and amoebicidal activity against T.vaginalis, E. histolytica and Giardia lamblia.
- It is also active against Blastocystis hominis, Balantadium coli, spirochaetes and anerobic streptococci.
- It is also active against :
- Anaerobic gram +ve bacilli:
Clostridium species and susceptible strains of Eubacterium - Anaerobic gram-negative bacilli:
Bacteroides like the group containing bacteroides fragilis. - Fusobacterium species
- Anaerobic gram +ve cocci: Peptococcus niger
- Peptostreptococcus species
- Campylobacter and helicobacter are also sensitive to metronidazole.
Resistance
Resistance can occur to metronidazole due to following properties in organisms:
- Diminished scavenging of O2, leading to increased amounts of oxygen locally. Thus metronidazole is not activated optimally leading to enhanced recycling.
- Episomally or chromosomally mediated nitroimidazole (nim) resistance genes have been found to be responsible for resistance in Bacteroides.
- Due to decreased ferrodoxin gene transcription there are reduced concentrations of ferrodoxin and PFOR.
- A functional mutation loss in rdxA gene which codes for NADPH nitroreductase which is not dependent on oxygen can lead to resistance in H. pylori.
Some microaerophilic and anerobic bacteria, Giardia lamblia, Trichomonas vaginalis, and Giardia intestinalis are resistant to metronidazole.
Pharmacokinetics
Orally administered metronidazole is readily absorbed. The t1/2 is ~8 hours. Some accumulation of the drug occurs if doses are repeated every 6-8 hours. Plasma protein binding is < 20%. Except placenta, metronidazole penetrates well into body tissues and fluids, including vaginal secretions, seminal fluid, saliva, breast milk, and CSF.
After an oral dose, >75% metronidazole is metabolized and is excreted through the kidney in urine. It is mainly metabolised in the liver by glucuronidation and oxidation. An acid and hydroxy metabolite are formed which are the major metabolites. More than half of the activity of metronidazole against trichomonas is exerted by the hydroxy metabolite. It also has a extended t1/2 of approximately twelve hours.
Therapeutic indications and dosage
1. Amoebiasis - Metronidazole is a first line drug for all forms of amoebic infection. For invasive dysentery and liver abscess-800 mg TDS (children 30-50 mg/kg/day) for 7-10 days. In serious cases of liver abscess 1 g may be infused i.v. slowly followed by 0.5 g every 8-12 hour till oral therapy is instituted. For mild intestinal disease - 400 mg TDS for 5-7 days.
2. Giardiasis - It is highly effective in a dose of 400 mg TDS for 7 days.
3. Trichomonas vaginitis – It is the drug of choice; 400 mg TDS for 7 days achieves nearly 100% cure. Nonspecific bacterial vaginosis also responds.
4. Anaerobic bacterial infections -Metronidazole is effective drug and is generally used along with gentamicin or cephalosporins. For serious cases i.v. administration is recommended: 15 mg/kg infused over 1 hour followed by 7.5/mg/kgevery6hours till oral therapy can be started with 400-800 mg TDS.
5. Pseudomembranous enterocolitis- Oral metronidazole 800 mg TDS preferred over vancomycin as it is more effective, more convenient, and less toxic.
6. Ulcerative gingivitis, trench mouth: 200-400 mg TDS (15-30 mg/kg/day) is quite effective because anaerobes are involved. Metronidazole /tinidazole are the drugs of choice for acute necrotizing ulcerative gingivitis, in which they are often combined with amoxicillin, tetracycline or erythromycin.
7. Helicobacter pylori gastritis/peptic ulcer - metronidazole 40 mg TDS or tinidazole 500 mg BD is frequently used along with amoxicillin/clarithromycin and omeprazole/pantoprazole/lansoprazole in triple drug 2 week regimens.
Drug Interactions
- A disulfiram like intolerance to alcohol occurs in some patients taking metronidazole as it inhibits aldehyde dehydrogenase enzyme.
- Oxidative metabolism of metronidazole is induced by the corticosteroid prednisolone, phenobarbitone, ethyl alcohol and rifampicin.
- Cimetidine inhibits hepatic metabolism of metronidazole.
- Metronidazole augments warfarin action by inhibiting its metabolism.
- It can reduce renal elimination of lithium.
Contraindications
- Prior history of hypersensitivity to Metronidazole or other nitroimidazole derivatives.
- Neurological disease, blood dyscrasias
- First trimester of pregnancy
- Chronic alcoholism
Mutagenesis, carcinogenicity, teratogenic effects
- Metabolites of metronidazole along with metronidazole has been found to cause mutagenesis in some bacteria and also known to give rise to tumours in higher doses in animals like mice.
- But there are no human clinical trials to prove this.
- Also there are no conclusive human clinical trials about the teratogenic effect of metronidazole and hence it should not be used in pregnancy and lactation.
Adverse effects
- Commonly seen side effects are decreased appetite, nausea, metallic taste, headache, cramp like pain in the abdomen, dryness of oral cavity.
- Vomiting, loose stools, rashes and transient neutropenia are seen infrequently.
- Accentuation of oral candidiasis can lead to inflammation of the tongue and oral cavity.
- Vertigo, giddiness, and very infrequently, convulsive episodes, encephalopathy, cerebellar ataxia and motor incoordination may lead to mandatory stoppage of metronidazole.
- Painful micturition and inflammation of the bladder can also be seen.
- Prolonged administration may cause peripheral neuropathy.